Common surgical procedures
Common gynaecological problems treated surgically
Endometrial polyps are noncancerous (benign) growths attached to the inner wall of the uterus (endometrium). They are localized overgrowth of cells/small tissue that vary in size from a few millimetres to some centimetres. There may be just one or many and they can be flat in shape or protrude with a long stem.
Although in most cases they are benign, in rare cases, they represent an early phase of cervical cancer and removing them helps reduce this risk. The risk of having malignant polyps is low in women of childbearing age but this risk increases with age. The presence of polys has been linked to difficulties to conceive.
A hysteroscopy, a minimally invasive surgical procedure, is the recommended procedure for the removal of any polyps. Removing the polys increases fertility and reduces miscarriages. Furthermore, it reduces the menstrual flow in women with heavy periods (menorrhagia) and they no longer have irregular bleeding.
Uterine fibroids also known as fibromyomas or leiomyomas, are the most common benign tumors that develop in the uterus. They consist of smooth muscle cells and connective tissue. They are usually hard, round, well-separated growths that can grow anywhere inside or on the uterus (Subserosal fibroids, grow on the outside of the uterus. Intramural fibroids grow inside the muscular wall of the uterus. Submucosal fibroids grow into the open space inside the uterus. Some fibroids become Pedunculated, having a stalk that attaches to the uterus.)
Their size range in size from seedlings (undetectable by the human eye) to bulky masses. You can have single or multiple fibroids.
It is unclear why they form, and research suggests they develop when oestrogen levels are higher (pregnancy, reproductive age, ovarian stimulation, and exogenous oestrogen intake) whereas they rarely develop in young women under 20 years while their size decreases after menopause.
In evaluating cases of uterine fibroids, the doctor considers multiple parameters such as the number, the location, and size of the fibroid as well as the age of the patient, fertility issues, and the presence of any symptoms.
Symptoms include heavy periods (menorrhagia) if they are submucosal or intracavitary, painful periods, pelvic pain if the fibroids are large in size, frequent urination if they put pressure on the bladder, and difficulty conceiving if they are intracavitary or large intramural.
When and if surgical removal is recommended, it is possible both laparoscopically and/or robotically. Submucosal or intracavitary fibroids can be removed via a hysteroscopy with precision and safety.
Hysteroscopic removal of submucosal fibroids increases fertility, reduces miscarriages and reduces the menstrual flow in women with heavy periods (menorrhagia).
An ovarian cyst is a sac or sac filled with fluid or other tissue that forms in or on the ovary. Ovarian cysts are an extremely common condition and may, to a small extent, pose a risk to a woman’s health.
Most women with ovarian cysts have no symptoms and this cyst is usually discovered by chance during a detailed gynecological examination or a routine ultrasound.
However, some cysts may cause symptoms which in some cases, may be severe. They include:
- Abdominal pain, pain during menstruation
- Feeling of heaviness in the genitals
- Severe pain from twisting or rupturing the cyst
- Swelling of the abdomen
- Menstrual disorders and abnormal uterine bleeding
- Endocrine disorders (menstrual disorders, early puberty in young girls, abnormality or absence of menstruation, masculinization).
When the ovarian cyst is characterized as a simple cyst and is less than 4 cm, then it is usually decided to simply monitor it with ultrasound. These are functional cysts and usually disappear within 2-3 months.
Cysts that do not disappear after 2-3 months usually need surgical removal. In some cases, it is clear through ultrasound evaluation that, even though the cyst is benign, such as endometrial cysts, dermoid cysts, ovarian cystadenoma, etc, it will not disappear on its own, and in such cases, surgical removal is done laparoscopically.
In case of suspicious ultrasound findings, surgical removal of the entire tumour is performed by laparoscopy. The tumor with the ovary is placed in a bag (laparoscopic endobag) and is carefully removed so that there is no spread of cancer cells in case of malignancy. A rapid biopsy is then performed and depending on the biopsy results, in some cases further specialized surgery may be required by the oncology team. This team includes several specialists, in addition to Dr. Kakkoura including a surgical oncologist, radiotherapists, and histopathologists. In case this group needs to be activated, the specialised doctors work closely with Dr. Kakkoura during and post-surgery to determine the treatment protocols that will be followed in each case.
Ectopic (Extrauterine) pregnancy is a complication of pregnancy in which the fetus attaches outside the uterus.
Most commonly an ectopic pregnancy occurs inside a fallopian tube (98% of cases). Diagnosing an ectopic pregnancy, especially in the early stages of pregnancy, is not
easy since the symptoms are the same as in any pregnancy including delayed menstruation, a positive pregnancy test, and some vague abdominal discomfort.
An ultrasound (to identify the location of the fetus) and a blood test to check the hormone levels of hCG confirm the ectopic pregnancy.
Early diagnosis is very important because the ectopic pregnancy can cause the woman’s fallopian tube to burst or rupture leading to abdominal bleeding and threatening the life of the woman.
The surgical treatment is done laparoscopically and involves removing the fetus and in the case of a fallopian tube pregnancy, removing the entire fallopian tube. It is also possible to inject cytostatics locally into the fetus inside the fallopian tube so that the fetus dies without removing the fallopian tube.
Under certain conditions and circumstances, a non-invasive, conservative treatment may be recommended with cytostatic medication.
Hysterectomy is one of the most common surgical procedures and involves the surgical removal of the womb (uterus). It can be partial (without the removal of the cervix) or total (with or without the ovaries and the fallopian tubes).
Once a woman has had a hysterectomy of any kind, she stops menstruating and cannot become pregnant.
Hysterectomy may be necessary in one of the following cases:
- Fibroids
- Endometriosis
- Adenomyosis
- Severe menorrhagia leading to anemia and not responding to other conservative treatments
- Uterine prolapse
- Endometrial, cervical, ovarian cancer
There are a few options for a hysterectomy:
- With laparotomy/Abdominal hysterectomy: incision in the abdomen and removal of the uterus.
- Vaginal hysterectomy: performed through an incision. This was the method of choice where there is a uterine prolapse (the cervix and uterus come down into the vagina or protrude out of the vaginal
entrance). Today, for the prolapse of the uterus, a robotic hysterectomy is also performed and recommended in order to support the vaginal stump at the same time with a grid on the sacrum – sacrocolpopexy. This technique is used to avoid the possibility of prolapse of the vaginal stump after vaginal hysterectomy. - Laparoscopic hysterectomy: this is performed with very small incisions in the abdomen to avoid large postoperative scars. Post-operative complications are significantly reduced. Only one day in hospital is required and the recovery is faster and painless, compared to the laparotomy.
- Robotic hysterectomy: What applies to the laparoscopic approach applies also to the robotic method. In addition, the surgeon has greater ease of surgical movements, a fixed camera, greater magnification, and sharpness, and the robotic surgeon has control – he handles both the camera and his tools.
Pelvic organ prolapse occurs when the muscles and ligaments supporting a woman’s pelvic organs weaken and the pelvic organs can drop lower in the pelvis, creating a bulge in the vagina (prolapse).
Some women with pelvic prolapse have no symptoms other than palpation of the prolapsed organ. Other women may experience pelvic or abdominal pain, pain on contact, heaviness in the genitals, frequent urination, urinary incontinence, bladder incontinence, urinary tract infections, abnormal vaginal discharge, and constipation.
Non-surgical treatments for pelvic prolapse include pelvic floor physical therapy and Kegel exercises and /or the use of vaginal ring pessary (medical device resembling the outer ring of a diaphragm used to support the pelvic area).
Reconstructive pelvic organ prolapse repair surgery aims to hold the organs in their correct locations. During surgery, the surgeon moves the organs back to their original positions and may implant surgical mesh support to keep the organs from moving. This process called Sacrocolpopexy is done using robotic or laparoscopic surgery.
Excellence in Minimally Invasive Gynaecology. A pioneering approach to pelvic organ prolapse.
Dr. Andri Kakkoura offers an advanced, minimally invasive solution using the En Place system. A refined, mesh-free, transvaginal technique designed to restore natural anatomy with precision and minimal downtime.
Introduced into her clinical practice in June 2025, and previously available only in Canada, the United States, and Israel, this innovative treatment is offered exclusively to her patients at American Medical Center.
Refined Technique. Faster Recovery. Exceptional Care.
• No abdominal incisions
• No synthetic mesh
• Procedure time ~ 30 minutes
• Local or general anesthesia
• Same-day discharge
Tailored to You
Every woman’s condition is unique.
Dr. Andri Kakkoura delivers a highly personalized treatment approach, combining clinical expertise with the latest advancements in minimally invasive gynaecology to ensure optimal outcomes.
Gynaecologic cancer is any form of cancer that starts in one of the woman’s reproductive organs and includes: Cervical, uterine, ovarian, vaginal, vulvar, and fallopian tube cancer. The most common is in the cervix, the endometrium, and the ovaries. It rarely concerns the fallopian tubes, the vagina, and vulva.
Each form of cancer has different symptoms and predisposing factors.
Women are encouraged to have annual gynaecological tests that include a gynaecological checkup, the Pap smear, and a gynaecological ultrasound, as treatment is most effective when the cancer is identified at an early stage.
Should a woman experience any of the following symptoms”, she should consult a gynaecologist :
- unusual vaginal bleeding, spots or discharge,
- abdominal pain,
- bloating, and
- unexplained weight loss
Depending on the location of the tumor and the stage of cancer, removal of the uterus and adjacent tissues (total hysterectomy) and/or removal of the ovaries and fallopian tubes may be suggested. Some cancers include pelvic lymph node dissection (endometrial cancer, ovarian cancer) and/or paraaortic lymph node dissection (ovarian cancer).
Within the framework of offering a complete and integrated treatment to patients dealing with gynecologic cancer, a special oncology team has been created which, in addition to Dr. Kakkoura, includes special oncologist surgeon Dr. Aggelos Sioutas, Director of the Oncology Surgery Clinic in Stockholm, who has extensive experience in cancer surgery. The team is furthermore supported by a specialist histopathologist, while there is full cooperation with the oncologists of the oncology centers in Cyprus.

How is appropriate surgery chosen to treat the various Gynaecological Conditions?
Treatment options for gynaecological conditions usually depend on the following factors:
- nature of the condition/disease.
- stage or severity of the condition.
- overall health of the patient.
- patient personal preferences. and
- age of the patient.
Hysteroscopy and laparoscopic surgical procedures as well as Robotic-assisted surgeries offer less post-surgery in-hospital care, faster patient recovery, less blood loss, fewer infections, and increased patient satisfaction.

Surgical Options
Any gynaecological condition which requires surgical intervention/procedure should be personalized and evaluated on a case-by-case basis so that the most appropriate surgical method may be chosen for each case.
Below we list the main invasive surgical procedures available:
The treatment of abnormalities of the cervix (polyps, fibroid tumours, diaphragms and adhesions) is done using a hysteroscope, a thin, lighted telescope-like instrument that is inserted into the woman’s uterus through the vagina. It allows the doctor to better examine the cervix and inside of the uterus and in case of operative hysteroscopy, small instruments are inserted through the hysteroscope to treat/correct the condition.
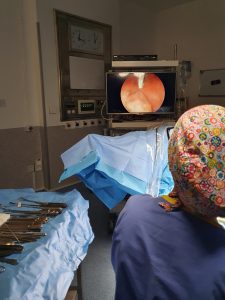
With open surgery, doctors make a large incision on the patient’s abdomen. The exact size of the incision will depend on the type of procedure being performed. Open surgery also called laparotomy, allows doctors to touch and feel key organs as they operate.
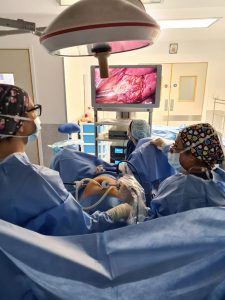
Laparoscopy is a minimally invasive surgical procedure by which the surgeon inserts small surgical instruments and a camera inside the abdomen via 3 small incisions (around 5cm each). Carbon dioxide is pumped into the woman’s abdomen and this further helps the surgeon see the organs more easily and operate.
It is possible to magnify the operating area on the screen and this provides an advantage over open surgery.
An additional advantage of laparoscopy over open surgery is the decreased recovery time as well as the lower likelihood of post-surgery inflammation.
Robotic surgery is an advanced laparoscopic procedure, only with an added layer of technology.
The surgery is conducted in a similar way as the laparoscopy in that both procedures use small incisions, a camera, and surgical instruments. In the case of robotic surgery, instead of holding and manipulating the surgical instruments, the surgeon performs the surgery via the console of the robotic surgery system*. The console gives high-definition, magnified, 3DHD views of the surgical area and allows the surgeon to controls a set of tiny “wristed” instruments. The console translates the surgeon’s hand movements in real-time, with instruments bending and rotating like a human hand but with a far greater range of motion for more precision, flexibility, and control than is possible with conventional techniques.
Thanks to robotic surgery, it is possible to perform many types of complex procedures which would have otherwise led to open surgery. For example:
- Myomectomy surgery to remove multiple, large or difficult to reach fibroids.
- A challenging hysterectomy due to the size of the womb or in case the patient has many pre-existing incisions from previous open surgeries.
- Pelvic organ prolapse repair surgery to support keeping the organs in place particularly after a hysterectomy.
- Specialised surgeries for cervical cancer and endometrial cancer with lymph node removal.
*Dr. Kakkoura is certified in robotic surgery using the da Vinci Robotic Surgery system.
Call Us
+357 22 476889
Reach Us
American Medical Center
215, Spyrou Kyprianou Avenue, 2047, Strovolos, Nicosia, Cyprus
Open Hours
Mon, Wed, Fri: 8:00 - 20:00
Tue: 8:00 - 17:00
Thu: 8:00 - 14:00
